The+Source
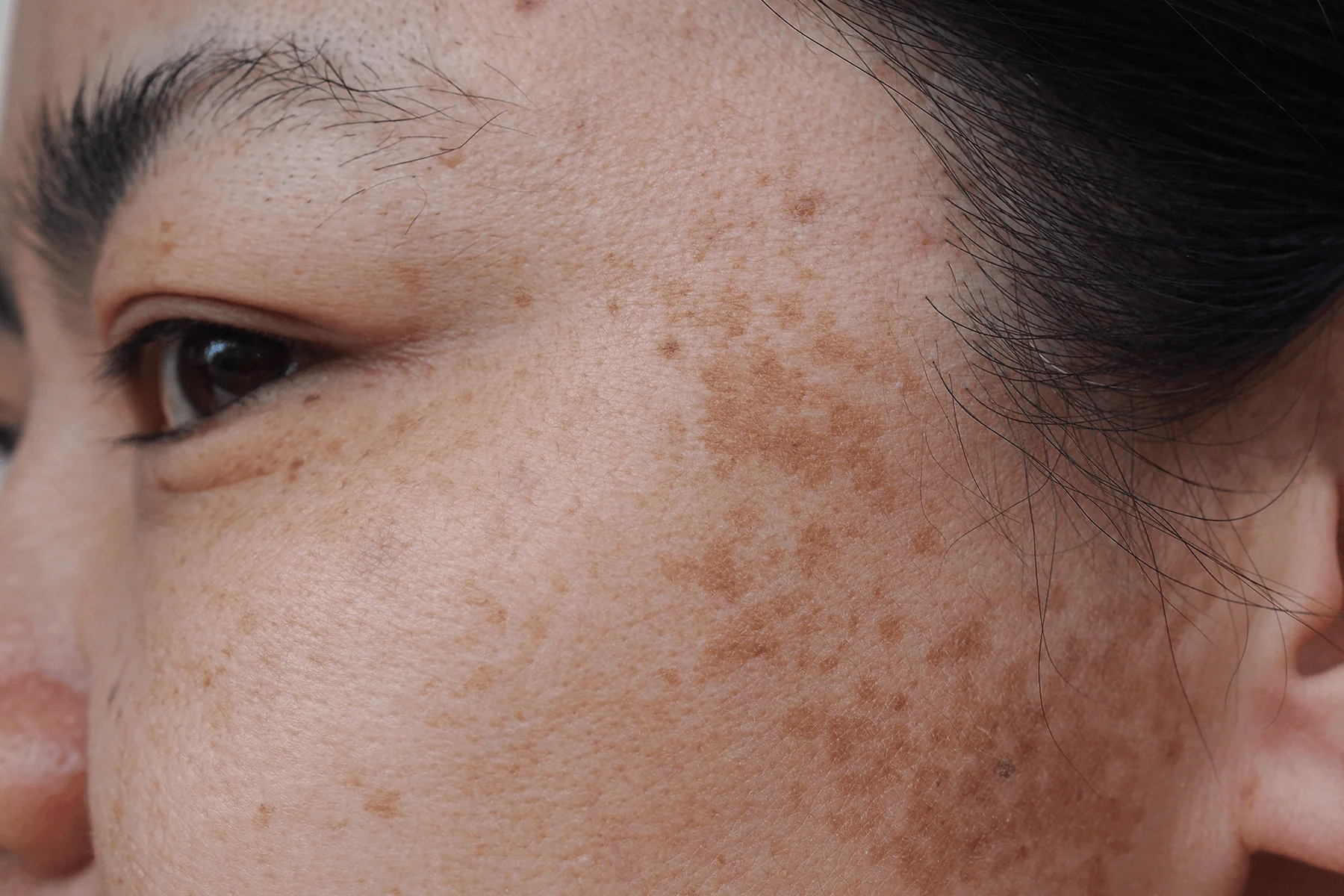
Pregnancy can bring about so many wonderful things (chief among them, a baby). But it can also welcome something else into your world – melasma. These areas of facial discoloration are often referred to as the “mask of pregnancy.” But you don’t have to be with child to suffer from this skin condition.
What is melasma?
Melasma is a form of hyperpigmentation that typically presents as brown patches on the face (most often on the forehead, cheeks, chin, and above the upper lip), although it can also appear on the arms or neck. While scientists don’t know exactly what causes melasma, they believe that hormones play a role since it’s primarily seen in women. (According to the American Academy of Dermatology, only 10 percent of melasma cases occur in men.) And while it’s estimated that between 15 and 50 percent of pregnant women get melasma, it can also afflict those on birth control pills or hormone replacement medication. Melasma is completely painless and sometimes disappears on its own (such as after pregnancy), but it is a chronic disorder, which means it’s more likely to be long-lasting (from three months to forever).
Causes of melasma & why does melasma happen?
Melasma seems to kick the melanocytes in the skin into overdrive. Melanocytes are the cells that produce melanin (aka pigment). Because the melanocytes in people with darker skin tones are already more active than those in individuals with lighter complexions, people with darker skin are more likely to develop melasma. That said, UV exposure makes melasma worse in anyone (which makes sense since UV exposure is pretty much bad news across the board). You can think your melasma has gone away, step outside unprotected, and find yourself right back where you started, in terms of having visible skin discoloration.
What are the types of melasma?
There are actually three kinds of melasma, although you’ll need a dermatologist and their Wood’s lamp (a device that emits black light to detect pigment irregularities, among other things) to know conclusively which one you have.
Epidermal melasma: This occurs in the top layer of skin (the epidermis). It’s typically dark brown, has crisp borders, and responds fairly well to treatment.
Dermal melasma: Located below the epidermis in the dermis, this kind of melasma is light brown or blue, has blurry edges, and—sadly—isn’t very responsive to treatments to eradicate it.
Mixed melasma: The most common of the three types, patches of mixed melasma are a combination of brown and blue that respond medium-well to efforts to erase them.
How to Treat Melasma
Resolving melasma requires a two-pronged approach: Fade the existing patches and prevent them from returning.
Treatment for current cases
Ingredients such as vitamin C and kojic acid can help remedy excess pigmentation by inhibiting tyrosinase (an enzyme in the melanocytes that triggers melanin formation). These are far preferable to other topical discoloration remedies, such as hydroquinone, that can be both irritating (causing hyperpigmentation to worsen in darker skin tones) and also have questionable safety profiles.
Gentle exfoliation via a chemical exfoliant like lactic acid can help slough off some of the discolored cells. The key word here is “gentle.” Anything that stings, burns, or otherwise irritates your complexion opens the floodgates to more melasma, which flares in response to harsh treatments. The Dr. Dennis Gross Alpha Beta Daily Peel Ultra Gentle formula offers the same key benefits of our universal and extra strength daily peels, but the addition of soothing, calming ingredients makes this peel accessible for everyone, even sensitive skin.
As noted above, some forms of melasma are incredibly stubborn. If this is the case with your skin, you may need to bring in the big guns (read: go to a dermatologist’s office). There, you can get a professional diagnosis of the procedure that’s right for your skin situation. They may suggest a chemical peel (although this is a stronger version of the exfoliation you may have tried at home, the risk that it will exacerbate your melasma is low as it’s performed in a controlled environment). Another option is a light-based procedure. This could be anything from IPL (Intense Pulsed Light), which is fairly mild, to a laser (such as a non-ablative fractionated one or a Q-switched version), that has a longer recovery period. Your dermatologist will determine the best course of action during your consultation.
To prevent future melasma flare-ups
Now that you’ve done all the work to get your melasma under control, you certainly don’t want it to return. Therefore, there are a few behaviors you’ll need to adopt going forward:
Maintain your skincare routine
If a topical ingredient worked for you to reduce your dark patches, don’t give it up once your melasma clears. You need to continue your successful regimen in order to keep pigmentation production in check.
SPF all day, every day
This is not news. You should already be applying SPF daily for a myriad of reasons. But add to that list the fact that UV exposure makes melasma infinitely worse. Most derms recommend a daily SPF of at least 30. Mineral or physical sunscreens are less irritating than the chemical kind, so they’re a wise option for the melasma-prone. Look for titanium dioxide or zinc oxide on the label. For extra protection, a broad-brimmed hat and sunglasses are also smart accessories when you step outside.
Skip waxing
This form of hair removal can cause both irritation and inflammation—essentially putting out the welcome mat for melasma. Talk to your dermatologist about the best alternative for your needs.
Discover Dr. Dennis Gross Skincare for All Your Skincare Needs
For more skincare tips from the experts at Dr. Dennis Gross, check out our blog’s newest content today. Shop the collection of Dr. Dennis Gross bestselling skincare backed by dermatologists.